A trauma-informed approach is defined as a strength-based program or system that realizes the widespread impact of trauma and understands potential paths for recovery, the signs and symptoms of trauma in clients, and others involved in the system; it then responds by integrating this knowledge into its practices and seeks to actively resist re-traumatization
I’m so glad that there has been a movement to implementing trauma-informed principles in all sorts of workplaces. Yoga classes, massage and physiotherapy, dental clinics, schools, and family lawyers have all made commitments to be more trauma-informed. While therapists may work with people who have experienced trauma, that does not always come with being trauma-informed. One would assume it’s part and parcel. That is not always the case, unfortunately. Further, sometimes the therapist is but their office or clinic does not work from a trauma-informed practice. Over the years of my work, I have both learned and implemented key principles and practices to ensure that my work is trauma-informed. For me, that includes doing what I can to help people I support feel safe and respected by me, that they are valued as the expert in their lives (versus me as a professional), their voice is empowered and have choices, as well as working from an intersectional anti-oppression framework: I work with compassion, collaboration and non-judgment. Being trauma-informed for me also includes knowing that everyone has a right to resilience and recovery/healing and trust is earned. I also know about the impact of trauma on people and have tools to assess for the symptoms.
As a Feminist Therapist for over 20 years, I strongly believe that being trauma-informed is deeply connected to my work: I’ve been a trauma-focused therapist for over 15 years. For instance, I know that people who identify as women (whether it is cis-gendered, trans or genderqueer, non-binary) experience gender-based violence at a far greater and disproportionate amount compared to their male peers. When I work with a new client, this informs my work – while she may be coming to me for support about adjusting to parenthood, she may have witnessed or experienced violence first-hand in her past. This may implicitly impact how she sees her role, workload, and role as a parent. Unresolved trauma lives and manifests in our bodies and lives in a way that keeps the trauma storied part of us activated.
Further, as a therapist who works with sexual violence, I also know that people who are giving birth who have a history of sexual assault may be very likely to experience triggers during pregnancy and birth – the birth process can be quite re-traumatizing in fact. This includes both the birth itself as well as the early postpartum period.
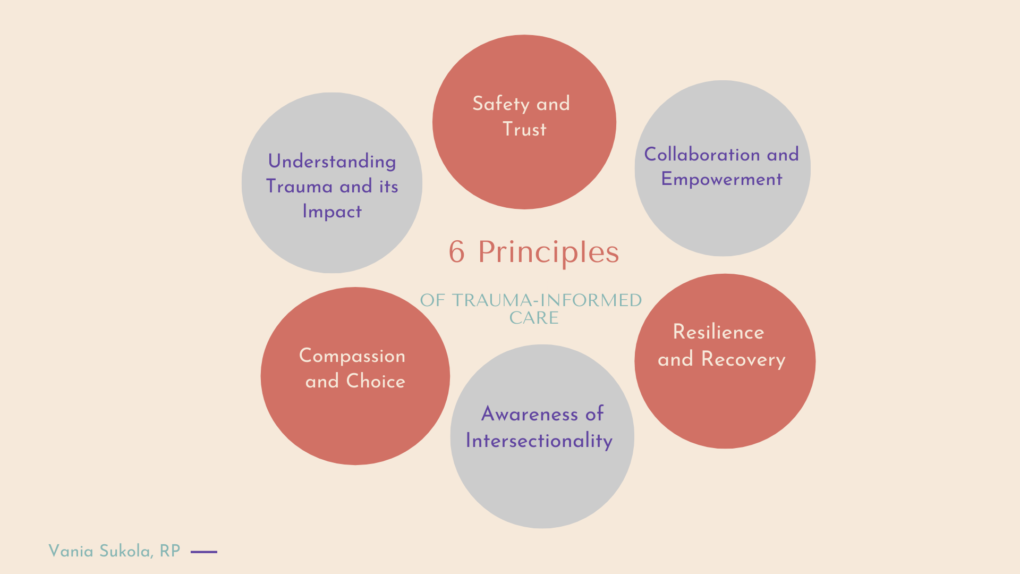
There are so many good models of trauma-informed care (TIC). I have put together this one with the 6 key principles that inform my work. For instance, I take the intake and assessment process slow. I don’t expect clients to share with me their history of trauma in the first 1-3 sessions (typically it’s seen as required information in order to get service). That disclosure should come with time, established trust and rapport, and the development of a relationship. I am a relational therapist – I value alchemy between us, I self-disclose my own lived experience at times (i.e my own miscarriage loss), and I am committed to work from a place of non-judgment and compassion. We build our work together on compassion and collaboration and they navigate how the sessions go – be it how and where they sit in the room, and what they want to talk about in session. As I’m trained in several therapy modalities, I also believe it’s important to use what is best for my clients, and would refer to someone else if it’s not the right fit.
Being a trauma therapist does not mean I expect to hear the trauma story itself. In fact, that may not happen at all. To me, being a trauma-informed trauma therapist means I work to help people access their resources (strategies that are physical, relational, spiritual, emotional and mental) so that they can find ways to integrate their trauma part (i.e traumatic birth experience) into their everyday life now, so that it doesn’t remain a fragmented part that still triggers them when it’s the anniversary/birthday. As trust is earned, it’s important to me that we build this connection slowly, and pace the trauma work so that people feel safe when they leave their session with me. While I don’t think anyone can guarantee a 100% safe place, I make it a practice to do my best to collaborate my clients.
Trauma-informed care for me also means that the person seeking my support is the expert in their own life – Clients are their own expert. I am just a guide that is there to support them. I don’t carry any expectations of my own. I also bear witness to the various social locations and how that can impact their healing i.e from birth trauma and the intersection if they are a racialized or otherwise marginalized person. I also overtly acknowledge my privilege as a white cis-gendered woman, who also has power as a psychotherapist. I make this intersection explicit in my work by naming the oppression for what it is, instead of minimizing. Making links to the systemic forms of discrimination is an important practice of TIC as it holds space for multiple truths instead of internalizing shame and guilt.
Working from a trauma-informed place also means that I am an advocate if the people i support need or request it. I share resources with you if part of your chosen healing journey includes taking legal action. There are great organizations and advocates that can support someone in their healing process. As big component of post-traumatic growth is when survivors advocate not only for themselves but others as well. That’s why movements like #metoo and Birth Monopoly are so powerful. It is inherently healing to feel interconnectedness with others who have similar stories. It’s part of my role and responsibility to share these resources with the people i support. I also bring it into my practice even when people don’t ask for it overtly – we don’t know what we don’t know is available as a resource.
Trauma-informed practice also includes how I take care of myself as I can be impacted by vicarious trauma. I have tools, activities, and regular practice of self-care. I also think it’s necessary to keep learning about my work, and push myself to be even better as a therapist. I seek out peer and clinical consultation and believe that all therapists need to do this, regardless of them being in practice for 5 or 25 years.
When you are seeking support from a therapist or practitioner, ask them what their definition of trauma-informed care is. If they don’t have one, that may be a sign that they are not thinking of the inherent impact and context of trauma. Not everyone works in a trauma-focused profession but if they are not at least trauma-informed in the practice, that means they are not keeping your safety and needs at their forefront of their work. Trauma does not have to be complex and Big T, but anyone who has lost a job, grieved the death of a loved one (including a pet), moved to a new city with no support, had a significant injury or illness have all experienced trauma that still lives in their body.
We deserve better. We deserve to get support that honours what our body knows. As Pat Ogden has so wisely shared, “the body always leads us home.”

