After giving birth to my first child, i knew when it came time to birth my second, i wanted it to look different. It took a lot of inner work first, as well as learning, unlearning, reflecting, and healing.
I did most of that on my own. When i had my first almost 12 years ago, i knew nothing of birth story healing work, let alone that a niche like perinatal mental health existed. When i had my son, an emergency c-section, i carried a lot of guilt and internalized stories that my body could not deliver a baby vaginally. I was told my body was too small and that it was failing to progress. I was told others weren’t surprised i had a c-section because I am small. What the actual fuck does that mean? I have come to hate these words and also learned to externalize that story. I have also given some of my son the responsibility – thanks for turning a bit too much, little one, i know you were trying to help. Your wee head just was too much for my swollen cervix after 30 hours of labour.
Move forward two years, and I’m pregnant again. I have already shared about the Birth Blessing Party. What i have not shared here is the actual home birth (after c-section, called HBAC for short). Now, after years of providing birth story healing work, and being so honoured to hear other’s stories, i have a deeper understanding and embodied trust in what i know to be a healing process to reclaim our birth stories.
What follows is the account of the birth of my youngest, layered with aspects of Polyvagal Theory, Somatic Therapies and more. I’m kind of excited that I made a connection to the gift of Polyvagal Theory to how birth happens. If you want to learn more about how i support other people to heal their birth stories, CHECK OUT THIS ARTICLE i wrote that unpacks it more. So, get ready for a self-professed Brain Geek Part of me coming out now and a brain-geek inspired birth story!…
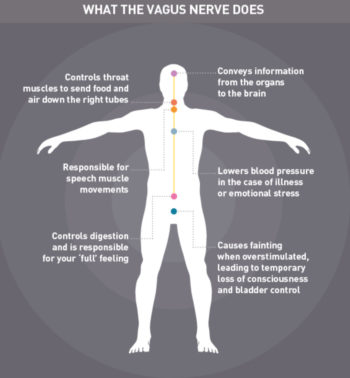
In case you haven’t heard of it, there has been a lot of (rightful) information about Polyvagal Theory. It is this wonderful nerve that acts as a pathway from our brain stem to our perineum. It provides all sorts of support to our body and how we react to the world. Since it so solidly lives in the pelvis as well as the brain, i love that I have seen how the theory can show up in action during childbirth. There are 3 stages of labour, just as there are 3 parts of Polyvagal Theory. I will go over them as i break down the story, but for now, as a summary: The Sympathetic Nervous System (the good ole Reptilian Brain) and the 2 parts of the Parasympathetic Nervous System (Ventral Vagus Nerve and Dorsal Vagus Nerve) make up Polyvagal Theory. Looking back at the birth of my child, i noticed that it helps me get a sense of why the supports and resources worked at the time, and what is also needed to help birthers in these various stages of labour.
As the theory is also linked to the Window of Tolerance (or ‘capacity’ as i like how it has been reframed), i would be remiss not to also include this great resource. Thanks to Dan Siegel and Pat Ogden, we now know that each of us has a threshold with what we can can take. On a given day, we may have a larger threshold (aka big bay window), and are more trying days, our window is as small as a peephole in an apartment building door. Knowing how the body responds to stress and danger helps us tend to where we are in the Window.
Please note, this is my own personal journey of birth; i know that not everyone can reclaim the power as i did. As a white cis-gendered femme woman, i have privilege that gives me access to these choices. I know not everyone has this same access and privilege, and am part of the movement to change that.
First things first, let’s start just before i went into labour. I had implemented a daily practice once i reached 36 weeks pregnant. It included a gentle yoga practice, hypnobirthing meditations, perineal massages with evening primrose oil, and eating all the good food. All of of this was to help me stay in my calm and rested zone, or Ventral Vagal Tone (soft and relaxed). Then, as i became 7 days “late”, i had to pivot as i had just been told that I would need to have a “well baby” ultrasound. I knew that would start the chain of events that would lead me away from my plan. So, that day, foreshadowing the birth, I did everything right to facilitate my child to be born without needing to go to that appointment. Spoiler alert: she was born 2 minutes before the appointment was supposed to happen.
That day, wanting to reclaim my power and agency, I made intentional choices. I had acupuncture and massage appointments, i had a solo date with a spicy dosa for lunch, i attended a La Leche League meeting with friends, and had a nap. I ate pineapple, cuddled with my boys, and had a family bath. You could say oxytocin was flowing.
It was when i stood up during this bath that I knew that the time had come.
 It’s Time! Baby is on Route
It’s Time! Baby is on Route
The sympathetic nervous system (SNS for short) is an essential part of our daily survival. It is where our reptilian brain helps us stay safe. Our Fight or Flight response lives here, protecting us from harm by either fleeing or fighting that which wants to cause us harm. This is the state of Hyperarousal in the Window of Tolerance (or Capacity) resource. When still within a regulated place, we can get a lot done as it motivates us into action. It is when we start to feel the flooding of emotions like overwhelm, anxiety or hypervigilance that things get dysregulated. If we can’t access the mode of activation that pushes us into action, the opposite realm of freeze (shutdown) or fawn (fix) happens. So, staying in the zone of movement helps us move the labour along. Hence the word ‘labour’ as the process is work.
The initial surge of contractions that initiate the start of labour are very similar to the autopilot response of flight or fight response. This early stage of labour is what helps the birther know that labour is starting; it’s like the brain kicks in and says ‘it’s time.’
It is here that we learn what we need to manage the new sensations in our body, where we make meaning of the surges. It is at this stage where we take stock of the process and see what is needed to keep safe and in control of the pain. It is also at this stage that we learn to discern fear of harm versus the worry of birth. It is no wonder we carry words like fear and pain with birth – pop culture stories on birth do not do this stage justice.
So, i worked on my breath, i paced, i swayed, i chatted. I moaned. I connected to my vagus nerve without even knowing. Moaning and swaying are beautiful remedies to get our body into the rest and calm it needs. They are directed rooted in the vagus nerve – no pun intended!
I also laughed and chatted with my partner, doula and midwife team. This sense of connection helped me stay grounded and centred, also a deep component of the vagus nerve.
Rest Time: Parasympathetic Dorsal Vagus Nerve
The dorsal vagus nerve lives in our back and lower body, hence ‘dorsal.’ This is the energy that is pulling us down, or into ‘down-regulation’ to help us get to a sense of rest. In the Window of Tolerance resource, this is the Hypoaroused state and can be quite supportive to get to a state of rest. It is where we have a nap, curl up in fetal pose, have luxurious baths, watch an old favourite show to pass the time. When still within the range of regulation, it serves us. It’s important to be attuned to this so that we have tools to stay within our range of capacity.
Sometimes, as in other times in our life, this part can overdo its job. It becomes overwhelmed and maybe a bit scared. In somatic therapy work, this feeling may show up as collapse, freeze, or shutdown when something hard on us needs to be tended to. It can manifest as feeling drained, scared, lonely or depressed. In labour, this is the time that our body starts to ask us to slow down but we are scared to ask for what it needs, helpers are telling us that we are not progressing fast enough, or our body does not feel heard that rest is vital here. Or, if this is the first birth for someone, they may be feeling like a fraud or unsure about what they are supposed to be feeling and are worried about disappointing their team. This is the pull of appeasement/fawning/fixing. I remember wanting to make sure the midwives were okay when i was having this hour-long shower!
While this story is about my second-born, during the birth of my son, before things changed and i was rushed to the hospital, this was the time that i listened to my favourite meditative playlist, watched Goonies, and went inward. When i was in labour with my daughter, this was the time that i had a long shower. It was so long that i drained most of the hot water. From 2-3AM, i was in the shower with the student midwife keeping me company, while my partner, doula, and primary midwife were making the birth pool. As the kitchen was the easiest place to do so, we found a way to fit it in. I will always associate water with soothing my tired, achy, and worried body. It was literally the balm I needed to soothe me.
In order to follow the flow of the birth, this next step officially happened here but it is actually a sympathetic nervous system moment: During birth, in the transition stage of getting past that beloved number of 7cm dilated, we are in this spot. We are starting to feel the shift inward. I will never forget that moment i thought my c-section scar split open, only to be validated that it was just my waters breaking and my baby reaching the right spot to descend. My fear was my inner Firefighter kicking in as it kept my worry brain active. And yet, it was overdoing its job – i was in fact in clear waters. Literally.
The Sweet Spot: The Ventral Vagus Nerve In Action
The Ventral Vagus Nerves lives in the front of our body. It is what helps us orient to our surroundings, access connection via our Social Engagement System. It acts as our Mirror of Safety and stems from the maternal co-regulation need. This nerve helps us pivot or neck to orient or centre ourselves. It is both Estrogen related and Oxytocin bonding. Just think of the importance of skin-to-skin care immediately after birht – that is for oxytocin to do its magic as it is flowing right there. Our vagus nerve is closest to the outside of our body at our chest – so this is why humming, buzzing like a bee, gargling, or stroking your chest in a gently rhythm are so helpful.

The birth pool plays a huge role in my birth story. Water is my Happy Place and creates the Glow my body needs to rest and feel safe. Being in it makes me recall my hypnobirthing and Birthing From Within mediations more easily. I also feel like a goddess in the water.
See that image? That’s my favourite place on Earth. It’s what i visualized during this birth and have come to use as my Happy Place Visual ever since. It was in the pool, when i looked at my doula Kim and saw the Full Moon outside the window. This moment defines everything for me.
There is this change that happens when we get to 10cm, also known as the sweet spot. While i can’t put it into words exactly, recalling this 9 years after the birth, i do remember the moment. I had just had that epic “oh my goodness, i just got there” moment, and locked eyes with my doula Kim. I saw the Full Moon outside the window, i heard the midwife team and my partner. This is what Stephen Porges calls Neuroception: when i relate to you and it is reciprocated. I know my sweet son was sleeping in bed right above us. I remember consciously connecting to him, even though he was not physically present in the room. I felt so entirely connected, seen, respected and attuned to my body.
Some things i learned that helped me stay present were:
– Somatic resources like a long bath, a lower back massage, or walking to get even just 5% more comfort in my body
– Have someone that is committed solely or intentionally to supporting you as the birther
– Pay attention to your edges where sits bone meets chair; do a mindful body scan
– Vagus Stroke exercise
– 5 senses of what to see, listen to, smell, feel, savour in my mouth
– Go deeper into my body – learn some meditation ahead of time, or ask your birth partner to help – things that help you notice interoception into fascia, bone, or muscle
– Notice songs or stories that resonate with you, ways to help you stay in the zone. It could be an embodied playlist or the story of Inanna.
It was then that i knew i could do this. It was at this moment that i entered my Self, no other parts were needed, and no other Part could step in as none had been here before. Having not reached this final stage of labour, i was so mindful and present with my body. I was not afraid anymore, and my lovely Manager part was able to step back and watch me in action.
It was recommended by the midwife that i get out of the pool to do a dilation check-in: i was at 10 cm, and that sensation i felt was my body’s way of letting me know that i was now ready to push. As i had not reached this stage last time, everything was new for me. I sat on a birth stool for a while and pushed. I transferred to the floor and pushed. I squeezed my partner’s hand and pushed. My son woke up sometime here and he saw his little sister’s crown. It was then that we knew that she was coming soon. So we called for back-up and my son’s best friend’s dad came and read to my son in the living room while we pushed. Incidentally, the story series about Franklin the turtle and hand-knit socks will forever be immortalized for me as a connection to the home birth. Listening to our friend gently read to our first-born was a balm for my body as it started to regulate and know it was safe.
I was in a zone while pushing, and to be honest, i don’t remember much of this part. I do recall that the Ring of Fire was the most searing pain i have ever felt. I have a vague memory that more came out of me than humanly possible. The animal in me overrode the Polite Lady Part who would have been mortified. And when sweet Miss M was birth earthside, she was not crying, and had a fist in the air. She was like, Hell Yes we did it. Yes we did.
Now each year, on her birthday, we do a dance on the spot where she was born.
So, why do we need to know about Polyvagal Theory or even the Window of Tolerance in reference to birth? When we know more about how our body and nervous system step in to help us under duress, a new experience or under threat and pain, this knowledge enables us to know what to do for our Self. Not all birthers can experience all three levels of Polyvagal – most may stay in SNS, and get some glimmers of the Vagal Parts. If you want to have an empowered, embodied and even orgasmic birth, this is where knowing how the theory relates to you makes the difference.
In an overwhelmed state, we freeze or collapse. Our bodies are built to follow this evolutionary path – if we can’t flee, we fight. When we discern that we can’t fight off the attack, we feign death or freeze. Some of us have access to the Fix/Fawn response first. Typically, when overwhelmed, we may shutdown and dissociate. We may lose track of time or focus. Anyone who utilizes the Fawn Response may use people-pleasing, minimizing their own needs, or make jokes to lessen what they are feeling and are afraid to ask form.

For instance, do you know if you respond to surprise/pain/fear in a Flight, Fight, Fix(fawn) or Freeze way? We don’t have to endure trauma in our life to have an instinctual response. Our nervous system kicks in to help us grapple with something tat is too much to bear or is overwhelming.
Fight – scream or roar like a jaguar, clench and claw your fingers or shake them, stomp; use ice cubes to cool you down
Flight – go for walks in first stage of labour, look for exits when in stage 3, move your neck, or rock your body; find your happy place
Fix/Fawn – talk to people in the room, use your voice and negotiate what you need; work on saying NO and know what your rights are, set boundaries, and tend to what you need, not hosting or tending to the others in the room.
Freeze – use warm water like a shower or birth pool; sway your body; find ways to stay warm on your periphery – your hands or your feet need to stay warm or grounded.
As our birth story is connected to the people who birthed before us, in our own lineage, we also carry those deep seeded experiences of pain, trauma, fear, and empowerment, awe, and wisdom. After having 2 very different births, i know that it is indeed possible to have an Empowered embodied mindful birth. And yet, that is not always available – As a white bodied cis-gendered woman, i also recognize how deeply seeded this assumption is that i have this right and access. Not everyone does. Structural racism and other forms of oppression keep this inherent birthright from all birthers. I also entirely believe that all births are natural, and the story matters. We matter. Birth Matters.


 I have mixed feelings about clubs. I never was a Girl Scout, in choir or on sports teams as a kid. I was a dancer though, but that doesn’t seem like the same kind of club or group like the others. For one thing, the rules and homogeneity that seemed to go along with it felt too forced. And just because one kid likes to play soccer, that doesn’t mean she likes the same music or food as another. And it felt like we had to be the same all the time, like Stepford Wives. I could be wrong though.
I have mixed feelings about clubs. I never was a Girl Scout, in choir or on sports teams as a kid. I was a dancer though, but that doesn’t seem like the same kind of club or group like the others. For one thing, the rules and homogeneity that seemed to go along with it felt too forced. And just because one kid likes to play soccer, that doesn’t mean she likes the same music or food as another. And it felt like we had to be the same all the time, like Stepford Wives. I could be wrong though.  Here’s why our well-intentioned comments about someone else’s experience can be problematic: it doesn’t take into account their potential birth trauma and how it’s linked to consent and body trust issues. We hear about birth trauma that relates to obviously upsetting experiences of injury or even infant death. But another type of birth trauma is one where the birther has their voice taken from them, and instead the medical expert is calling all the shots. When some of us have experienced sexual violence and later in life get pregnant, this new experience can bring up former body memories and triggers.
Here’s why our well-intentioned comments about someone else’s experience can be problematic: it doesn’t take into account their potential birth trauma and how it’s linked to consent and body trust issues. We hear about birth trauma that relates to obviously upsetting experiences of injury or even infant death. But another type of birth trauma is one where the birther has their voice taken from them, and instead the medical expert is calling all the shots. When some of us have experienced sexual violence and later in life get pregnant, this new experience can bring up former body memories and triggers.  My eldest child was born 8 years ago this week. Looking back on the birth, i credit the experience i had personally with what motivated me to do the work i do. It wasn’t the birth i wanted, and while i have moments of it that i treasure to this day, parts of it were really scary and it’s taking me time to heal from them. I know i’m one of the lucky ones and my birth trauma is my own story. I also know that i have more tools on hand to heal and delve into the trauma than most of us have. Please read on only if you want to.
My eldest child was born 8 years ago this week. Looking back on the birth, i credit the experience i had personally with what motivated me to do the work i do. It wasn’t the birth i wanted, and while i have moments of it that i treasure to this day, parts of it were really scary and it’s taking me time to heal from them. I know i’m one of the lucky ones and my birth trauma is my own story. I also know that i have more tools on hand to heal and delve into the trauma than most of us have. Please read on only if you want to.  Between 5AM and 11AM my care had to be transferred over to an OB doc. This was devastation #1. I so admired my team of midwives and felt so connected to them, having to be transferred felt like a betrayal even though my Wise Mind knew it was necessary. The doc did not have the same bedside manner or a trauma-informed framework. Ironically, it was the anesthesiologist that helped me get through the discussion that i ‘needed’ to have an emergency C-section. I remember being told that my son’s head was stuck and i was too swollen to give birth vaginally. I remember thinking that in his excitement to meet me, my baby turned a bit too much and got stuck. I remember the pain before the epidural and thinking ‘there is no way that those of us that birth can do this.’ The pain was surreal.
Between 5AM and 11AM my care had to be transferred over to an OB doc. This was devastation #1. I so admired my team of midwives and felt so connected to them, having to be transferred felt like a betrayal even though my Wise Mind knew it was necessary. The doc did not have the same bedside manner or a trauma-informed framework. Ironically, it was the anesthesiologist that helped me get through the discussion that i ‘needed’ to have an emergency C-section. I remember being told that my son’s head was stuck and i was too swollen to give birth vaginally. I remember thinking that in his excitement to meet me, my baby turned a bit too much and got stuck. I remember the pain before the epidural and thinking ‘there is no way that those of us that birth can do this.’ The pain was surreal. 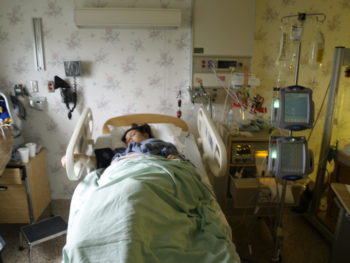 My baby was born that Sunday afternoon, just as the Pride parade was starting. We saw a rainbow out of our minuscule window. It overlooked the lake and i worked hard to rid the delivery/surgery room from my mind. My baby and i worked hard on our latch, our breastfeeding, our bonding. We worked on our rest and healing. We stayed at the hospital for 3 days. We stayed together in our small shared room. We saw other families come in and out. I worked on getting to the bathroom. Devastation #7 is learning the incredible feat of getting out of bed to walk across the room to pee. Devastation #8 is being told i had to work on a poo before leaving the hospital. Yikes, how was that supposed to happen. Devastation #9 is being told that my baby wasn’t latching so wasn’t getting what he needed – i have had my period and big boobs since the age of 9, if nothing else my body was born to breastfeed! He had one dose of formula to get us through that night shift with that 1 nurse. And then i worked my butt off to get him to latch.
My baby was born that Sunday afternoon, just as the Pride parade was starting. We saw a rainbow out of our minuscule window. It overlooked the lake and i worked hard to rid the delivery/surgery room from my mind. My baby and i worked hard on our latch, our breastfeeding, our bonding. We worked on our rest and healing. We stayed at the hospital for 3 days. We stayed together in our small shared room. We saw other families come in and out. I worked on getting to the bathroom. Devastation #7 is learning the incredible feat of getting out of bed to walk across the room to pee. Devastation #8 is being told i had to work on a poo before leaving the hospital. Yikes, how was that supposed to happen. Devastation #9 is being told that my baby wasn’t latching so wasn’t getting what he needed – i have had my period and big boobs since the age of 9, if nothing else my body was born to breastfeed! He had one dose of formula to get us through that night shift with that 1 nurse. And then i worked my butt off to get him to latch.